Opioid Addiction Treatment in Chennai: A Modern, Evidence-Based Approach
 Opioid addiction is no longer a distant public health issue—it is increasingly seen in urban clinical practice, including in Chennai. From prescription opioid misuse to heroin and injection drug use, the spectrum is broad and often hidden.
Opioid addiction is no longer a distant public health issue—it is increasingly seen in urban clinical practice, including in Chennai. From prescription opioid misuse to heroin and injection drug use, the spectrum is broad and often hidden.
The good news is this: effective, evidence-based treatment exists—and recovery is very much possible.
Understanding Opioid Addiction
Opioids act on the brain’s reward system, producing relief, euphoria, and eventually dependence. Over time, the brain adapts, and stopping opioids leads to:
- Severe withdrawal symptoms
- Intense cravings
- High relapse risk
This is why opioid addiction is best understood not as a “habit,” but as a chronic, relapsing brain disorder.
Why “Cold Turkey” Often Fails
Many patients and families initially attempt abrupt cessation (“cold turkey”). While well-intentioned, this approach has serious limitations:
- Severe withdrawal distress → poor adherence
- Relapse rates are very high
- Increased overdose risk after relapse (due to loss of tolerance)
Modern psychiatry strongly favors Medication-Assisted Treatment (MAT) over unaided detoxification.
The Gold Standard: Buprenorphine-Based Treatment (OST)
What is Buprenorphine?
Buprenorphine is a partial opioid agonist, commonly prescribed as a sublingual combination with naloxone (to reduce misuse potential).
Popular formulations in India include:
- Addnok
- Qudict
These are widely used in clinical and deaddiction settings across the country.
How Buprenorphine Works
Buprenorphine occupies opioid receptors in a unique way:
- Reduces withdrawal symptoms
- Suppresses cravings
- Produces a “ceiling effect” → beyond a point, increasing dose does not increase respiratory depression
This makes it significantly safer than full opioid agonists.
The addition of naloxone:
- Prevents misuse via injection
- Enhances safety in real-world settings
Why Buprenorphine is Considered Safe
- Lower overdose risk due to ceiling effect
- Stable receptor activity → avoids highs and lows
- Allows functional recovery (patients can work, engage with family, and rebuild life)
- Proven harm reduction → reduces infections, injection use, and mortality
It is important to be precise:
Buprenorphine is not “risk-free,” but when used under medical supervision, it is one of the safest and most effective treatments available for opioid dependence.
Evidence from India
India has a substantial burden of opioid dependence:
- ~1 million people are dependent on opioids (National survey data)
Clinical studies and national program data show:
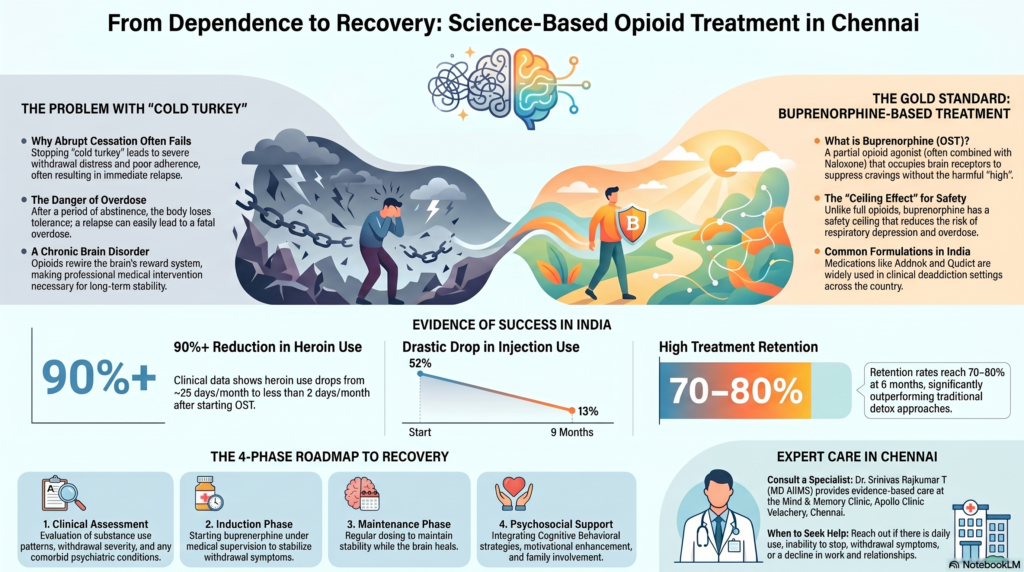
- Heroin use reduced from ~25 days/month to <2 days/month after OST
- Injection drug use reduced from ~52% to 13% within 9 months
- Retention rates ~70–80% at 6 months, significantly better than most other approaches
Buprenorphine-based OST is also a core component of the National AIDS Control Programme (NACO), emphasizing its role in harm reduction.
What Treatment Looks Like in Practice
A structured opioid addiction treatment plan typically includes:
1. Assessment
- Substance use pattern
- Withdrawal severity
- Comorbid psychiatric conditions
2. Induction Phase
- Starting buprenorphine under supervision
- Stabilizing withdrawal
3. Maintenance Phase
- Regular dosing
- Gradual psychosocial stabilization
4. Psychosocial Interventions
- Motivational enhancement
- Cognitive behavioral strategies
- Family involvement
Addressing Common Myths
“Isn’t this replacing one addiction with another?”
No.
Buprenorphine is a controlled, therapeutic medication that stabilizes the brain—not a substance that produces harmful intoxication patterns.
“Can I stop once I feel better?”
Premature discontinuation increases relapse risk. Duration is individualized.
“Is it only for severe cases?”
It is particularly useful in moderate to severe opioid dependence, especially with:
- Injection drug use
- Repeated relapses
- Failed detox attempts
Opioid Addiction Treatment in Chennai
Chennai now has access to structured, evidence-based deaddiction care, including:
- Buprenorphine–naloxone therapy (OST)
- Psychiatric evaluation and monitoring
- Integrated psychosocial interventions
Early treatment significantly improves outcomes—not just medically, but socially and functionally.
When to Seek Help
Consider professional help if there is:
- Daily opioid use
- Inability to stop despite attempts
- Withdrawal symptoms on stopping
- Injection drug use
- Decline in work, relationships, or health
Final Word
Opioid addiction is serious—but it is treatable.
The shift from willpower-based approaches to science-based care has transformed outcomes worldwide—and the same is now available in Chennai.
Recovery is not just about stopping a substance.
It is about restoring function, dignity, and stability.
About the Author
Dr. Srinivas Rajkumar T, MD (AIIMS, New Delhi), DNB, MBA (BITS Pilani)
Consultant Psychiatrist & Neurofeedback Specialist
Mind & Memory Clinic, Apollo Clinic Velachery (Opp. Phoenix Mall)
✉ srinivasaiims@gmail.com 📞 +91-8595155808